Posts Tagged hand function
[Abstract + References] The usefulness of assistive soft robotics in the rehabilitation of patients with hand impairment: A systematic review
Posted by Kostas Pantremenos in Paretic Hand, REHABILITATION, Rehabilitation robotics on March 26, 2024
Abstract
Introduction
Loss of hand function causes severe limitations in activity in daily living. The hand-soft robot is one of the methods that has recently been growing to increase the patient’s independence. The purpose of the present systematic review was to provide a classification, a comparison, and a design overview of mechanisms and the efficacy of the soft hand robots to help researchers approach this field.
Methods
The literature research regarding such tools was conducted in PubMed, Google Scholar, Science Direct, and Cochrane Central Register for Controlled Trials. We included peer-reviewed studies that considered a soft robot glove as an assistive device to provide function. The two investigators screened the titles and abstracts, then independently reviewed the full-text articles. Disagreements about inclusion were resolved by consensus or a third reviewer.
Results
A total of 15 articles were identified, describing 210 participants (23 healthy subjects). The tools were in three categories according to their actuation type (pneumatic system, cable-driven, another design). The most critical outcomes in studies included functional tasks (fourteen studies), grip strength (four studies), range of motion (ROM) (five studies), and user satisfaction (five studies).
Discussion
Function and grip parameters are the most common critical parameters for tests of hand robots. Cable-driven transmission and soft pneumatic actuators are the most common choices for the actuation unit. Radder et al. study had the highest grade from other studies. That was the only RCT among studies.
Conclusion
Although few soft robotic gloves can be considered ready to reach the market, it seems these tools have the potential to be practical for people with a disability. But, we lack consistent evidence of comparing two or more soft robot gloves on the hand functions. Future research needs to assess the effect of soft robotic gloves on people with hand disorders with more populations.
Introduction
Over sixty million people suffer from hand disabilities globally (Lawrence et al., 2001; Organization and Society, 2013). Hand function recovery is crucial for the independence of people with disability (Almenara et al., 2017). Hand robots are one of the methods that are growing recently because of increasing the patient’s independence (Gopura et al., 2011). Soft robots and exoskeletons are two available benches for rehabilitation robots. High weight, bulky, complex, and limited interaction with an environment are some of the limitations of the exoskeletons (Gopura et al., 2016; Jiryaei et al., 2021). The exoskeletons are expensive and non-portable, which restricts the rehabilitation process at home. Hence, they need to develop lightweight and wearable robots (Cappello et al., 2018; Trivedi et al., 2008).
Soft robots are one of the newest and most innovative technological devices. These tools allow interaction between the execution of motions and the intentions of the tool and the users (Kazerooni, 2005; Pons et al., 2008). Clinical studies showed that users who used soft robotics during rehabilitation programs significantly improved hand motor functionality compared to patients without soft robots (Ueki et al., 2010).
Recently, many research groups have begun to develop and evaluate robotic gloves with soft and flexible materials (e.g., cable-driven, fluidic soft actuators, and soft pneumatic actuators) (Bardi et al., 2022; Trivedi et al., 2008). Soft robots provide more degrees of freedom, more safety, less weight, and less complexity than exoskeletons. In addition, the soft robots are suitable for delicate and sensitive movements and improve activities of daily living (ADL) with the hand (Diftler et al., 2014; Heo et al., 2012; Kadowaki et al., 2011; Polygerinos et al., 2015; Trivedi et al., 2008).
Using soft materials enables a structure without joints, which resolves the problem of aligning human finger joints with a rigid exoskeleton (Sarakoglou et al., 2016). This concept of a wearable soft-robotic glove allows low-performance users to employ their hands in ADL. It may even reduce the need for healthcare professionals and is thought to improve hand-function users’ independence in performing ADL (Radder et al., 2019).
In a systematic review, Bardi et al., assessed sixty-nine soft robots for the upper limb (105 articles) (Bardi et al., 2022). Although this review included a wide of soft robots for upper limbs, the researchers reviewed the studies related to technical points and did not consider clinical tests. In a narrative review, the clinical outcomes of the soft robots were reviewed, but only papers with SCI participants were selected (Cardoso et al., 2022). To the best of our knowledge, a comprehensive review of the topic with a clinical view needs to be included. Thus, this systematic review provides a classification, a comparison, and a design overview of mechanisms and the efficacy of the soft glove robots to help researchers approach this field. We reviewed these outcomes outcome measures functional tasks, grip and pinch strength, ROM, and user satisfaction, in the present study.
Section snippets
Search strategy
This systematic review was conducted according to the guidelines of the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) statement (Mark Vrabel, 2015) and registered with the PROSPERO database. The search strategy was based on the Population Intervention Comparison Outcome (PICO) method and included all relevant articles published from January 2005 to April 2022. Do studies of hand robots could be benefit for researchers and clinicians? To answer this question a
Description of the studies
The present study restricted the research to papers written in English and published from January 2005 to April 2022 (see Fig. 1). The search strategy yielded 874 articles. After a full review of the articles, 15 met the inclusion criteria. This review summarizes the results of studies that evaluated soft robotic gloves on patients with hand impairment. The researchers modified the Downs and Black scale to 15 items. Four papers received a maximum score (a score of 12), and the six papers
Discussion
The present study demonstrates soft robots will have a very high potential in the near future. However, this area needs more strong evidence and clinical tests. This review’s results amplify the effect of clinical tests of soft robot gloves. The main applications for which these tools have been developed are related to the assistance of disabled people. Function and grip parameters are the most common critical parameters for tests of hand robots. From a technical view, cable-driven transmission
Conclusion
In conclusion, this study confirms that soft robots might show very high potential, but they have yet to reach the market. This review could infer no reports with long effects of using soft devices on ADL and the quality of life of disabled people. Thus, clinical trials are needed to assess the effectiveness of soft hand robots and identify the needs of disabled people who can benefit the most from these types of tools. Overall, soft robots can be a window of hope for them. Hopefully, soon
Clinical relevance
- •Soft robots may improve grip, reduce limitations and increase function.
- •Soft robots may benefit by increasing the quality of life for people with disability in hand.
References (39)
- R. Gopura et al.Developments in hardware systems of active upper-limb exoskeleton robots: a reviewRobot. Autonom. Syst.(2016)
- Z. Jiryaei et al.Development and feasibility of a soft pneumatic-robotic glove to assist impaired hand function in quadriplegia patients: a pilot studyJ. Bodyw. Mov. Ther.(2021)
- M. Almenara et al.Usability test of a hand exoskeleton for activities of daily living: an example of user-centered designDisabil. Rehabil. Assist. Technol.(2017)
- E. Bardi et al.Upper limb soft robotic wearable devices: a systematic reviewJ. NeuroEng. Rehabil.(2022)
- L. Cappello et al.Assisting hand function after spinal cord injury with a fabric-based soft robotic gloveJ. NeuroEng. Rehabil.(2018)
- L.R. Cardoso et al.Soft robotics and functional electrical stimulation advances for restoring hand function in people with SCI: a narrative review, clinical guidelines and future directionsJ. NeuroEng. Rehabil.(2022)
- M. Diftler et al.RoboGlove-A robonaut derived multipurpose assistive device
- S.H. Downs et al.The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventionsJ. Epidemiol. Community(1998)
- H.C. Fischer et al.Use of a portable assistive glove to facilitate rehabilitation in stroke survivors with severe hand impairmentIEEE Trans. Neural Syst. Rehabil. Eng.(2015)
- L. Ge et al.Design, modeling, and evaluation of fabric-based pneumatic actuators for soft wearable assistive glovesSoft Robot.(2020)
View more references
[Abstract] An exoskeleton rehabilitation system to train hand function after stroke
Posted by Kostas Pantremenos in Paretic Hand, REHABILITATION, Rehabilitation robotics on April 13, 2023
Abstract
| Stroke is a leading cause of disability in adults. Notably, about 75% of stroke survivors have upper limb damage, which greatly reduces the quality of life of the patient after recovery. The current routine rehabilitation recommendation is repetitive functional training (exercise-based training) to promote nervous system recovery, and then realize exercise rehabilitation. The cost, efficiency and success rate of traditional treatment methods are unstable due to various factors such as the professional level of therapists, the time required and the workload of therapists. In the case, rehabilitation robot-assisted therapy brings a new direction for the rehabilitation of stroke hemiplegia. In this paper, a new type of hand rehabilitation robot is designed based on the physiological structure of fingers, which is used to assist stroke patients in different stages of finger movement rehabilitation training. It can help the patient to practice grasp adduction and abduction repeatedly, reducing the burden on the patient. Secondly, in this paper, the degrees of freedom and movement of each finger joint are analyzed and calculated. Through modelling and finite element analysis based on Solid works to simulate the stress changes of exoskeleton in different rehabilitation stages, a model suitable for different stages of rehabilitation training is put forward. |
[WEB] Spinal Cord Stimulation Restores Post-Stroke Arm, Hand Function
Posted by Kostas Pantremenos in Paretic Hand on March 22, 2023
For the first time, researchers have used electrical stimulation of the cervical spinal cord to immediately restore arm and hand movement in two patients with chronic moderate-to-severe upper limb paresis.

A research participant gives a thumbs up while holding a fork with a piece of steak with her affected arm.
The results provide “promising, albeit preliminary, evidence that spinal cord stimulation could be an assistive as well as a restorative approach for upper-limb recovery after stroke,” first author Marc P. Powell, PhD, Reach Neuro Inc., Pittsburgh, Pennsylvania, and colleagues wrote.
The findings were published online February 20 in Nature Medicine.
Top Cause of Paralysis
“Stroke is the largest cause of paralysis in the world,” with nearly three quarters of patients with stroke experiencing lasting deficits in motor control of their arm and hand, co-senior study author Marco Capogrosso, PhD, assistant professor of neurological surgery at the University of Pittsburgh, Pittsburgh, Pennsylvania, said during a press briefing.
Stroke can disrupt communication between the brain and the spinal cord, leading to motor deficits in the arm and hand. However, below the lesion, the spinal circuits that control movement remain intact and could be targeted to restore function, Capogrosso noted.
Spinal cord stimulation has shown promise in promoting long-lasting recovery of leg motor function in patients with spinal cord injury; but until now, it’s been largely unexplored for upper-limb recovery.
In this “first-in-human” study, the investigators percutaneously implanted two linear leads in the dorsolateral epidural space targeting neural circuits that control arm and hand muscles in two patients.
One of the patients was a woman (age, 31 years) who had experienced a right thalamic hemorrhagic stroke secondary to a cavernous malformation 9 years before enrolling in the pilot study.
The other patient was a woman (age, 47 years) who experienced a right ischemic middle cerebral artery (MCA) stroke secondary to a right carotid dissection, resulting in a large MCA territory infarct 3 years before entering the study.
In both patients, continuous stimulation of the targeted neural circuits led to significant and immediate improvement in arm and hand strength and dexterity. This enabled the patients to perform movements that they couldn’t perform without spinal cord stimulation.
The process also enabled fine motor skills, such as opening a lock and using utensils to eat independently — tasks that the younger woman had not been able to do for 9 years.
“Perhaps even more interesting, we found that after a few weeks of use, some of these improvements endure when the stimulation is switched off, indicating exciting avenues for the future of stroke therapies,” Capogrosso said in a news release.
No serious adverse events were reported.
‘Easily Translated’
Capogrosso said that, thanks to years of preclinical research, the investigators have developed a practical, easy-to-use stimulation protocol adapting existing clinical technologies that “could be easily translated to the hospital and quickly moved from the lab to the clinic.”
The researchers noted, however, that further studies in larger cohorts will be required to validate the safety and efficacy of this approach.
They are currently working with more patients with stroke to fine-tune placement of the leads and stimulation protocol, as well as determine which patients are best suited for the approach.
“Creating effective neurorehabilitation solutions for people affected by movement impairment after stroke is becoming ever more urgent,” co-senior author Elvira Pirondini, PhD, assistant professor of physical medicine and rehabilitation at the University of Pittsburgh, said in the release.
“Even mild deficits resulting from a stroke can isolate people from social and professional lives and become very debilitating, with motor impairments in the arm and hand being especially taxing and impeding simple daily activities, such as writing, eating, and getting dressed,” she added.
This research was funded by the National Institutes of Health BRAIN Initiative, with additional research support provided by the Department of Neurological Surgery and the Department of Physical Medicine and Rehabilitation at Pitt, and the Department of Mechanical Engineering and the Neuroscience Institute at Carnegie Mellon University. Three investigators have financial interests in Reach Neuro, Inc., which has an interest in the technology being evaluated in this study.
Nature Med. Published online February 20, 2023. Abstract.
[Abstract] Perspectives and expectations of stroke survivors using egocentric cameras for monitoring hand function at home: a mixed methods study
Posted by Kostas Pantremenos in Paretic Hand on October 14, 2022
Abstract
Purpose
Most stroke survivors have remaining upper limb impairment six months after stroke and require additional rehabilitation and help from family members to enhance their performance of daily activities. First-person (egocentric) video has been proposed to capture the activities of daily living (ADLs) of stroke survivors in order to assess their hand function at home. This study explored the experiences and expectations of stroke survivors regarding the use of egocentric cameras in daily life for rehabilitation applications.
Methods
Twenty-one chronic stroke survivors recruited for the study were asked to record three sessions of 1.5 h of video of their ADLs at home over two weeks. Their experiences and expectations after completing the recordings were discussed using a structured questionnaire and a semi-structured interview. The questionnaire and interview data were analysed using descriptive statistics and content analysis, respectively. The results were further integrated using a mixed methods analysis for mutual explanation and elaboration.
Results
The themes generated were Camera Usability, Privacy Concerns Related to Home Recordings, Future Use of the Camera in Public, and Information Usefulness. The participants perceived that the camera was easy to use, the information obtained from the recordings was beneficial, and no major concerns about recording at home. A discreet camera and a solution to privacy issues were prerequisites to recording tasks in public.
Conclusions
There was high acceptance among stroke survivors regarding the use of wearable cameras for rehabilitation purposes in the future. Concerns to be managed include discomfort, self-consciousness, and the privacy of others.
- Implications for rehabilitation
- The egocentric camera was easy for the stroke survivors to use at home. However, they expressed a preference for cameras to be less noticeable and lighter in the future to minimize self-consciousness and discomfort.
- Expectations for future use of an egocentric camera for upper limb rehabilitation at home from the perspectives of stroke survivors included receiving feedback on their hand function in daily life and guidance on how to improve function.
- Privacy concerns of stroke survivors regarding recording activities of daily living were mostly avoidable by planning in advance. However, some personal hygiene tasks and virtual meetings were recorded by accident. A checklist of common activities that may raise privacy issues can be provided along with the camera to serve as a reminder to avoid these issues.
[Abstract] SSVEP-Based Brain Computer Interface Controlled Soft Robotic Glove for Post-Stroke Hand Function Rehabilitation
Posted by Kostas Pantremenos in Paretic Hand, Rehabilitation robotics on June 27, 2022
Abstract:
Soft robotic glove with brain computer interfaces (BCI) control has been used for post-stroke hand function rehabilitation. Motor imagery (MI) based BCI with robotic aided devices has been demonstrated as an effective neural rehabilitation tool to improve post-stroke hand function. It is necessary for a user of MI-BCI to receive a long time training, while the user usually suffers unsuccessful and unsatisfying results in the beginning. To propose another non-invasive BCI paradigm rather than MI-BCI, steady-state visually evoked potentials (SSVEP) based BCI was proposed as user intension detection to trigger the soft robotic glove for post-stroke hand function rehabilitation. Thirty post-stroke patients with impaired hand function were randomly and equally divided into three groups to receive conventional, robotic, and BCI-robotic therapy in this randomized control trial (RCT). Clinical assessment of Fugl-Meyer Motor Assessment of Upper Limb (FMA-UL), Wolf Motor Function Test (WMFT) and Modified Ashworth Scale (MAS) were performed at pre-training, post-training and three months follow-up. In comparing to other groups, The BCI-robotic group showed significant improvement after training in FMA full score (10.05±8.03, p=0.001), FMA shoulder/elbow (6.2±5.94, p=0.0004) and FMA wrist/hand (4.3±2.83, p=0.007), and WMFT (5.1±5.53, p=0.037). The improvement of FMA was significantly correlated with BCI accuracy (r=0.714, p=0.032). Recovery of hand function after rehabilitation of SSVEP-BCI controlled soft robotic glove showed better result than solely robotic glove rehabilitation, equivalent efficacy as results from previous reported MI-BCI robotic hand rehabilitation. It proved the feasibility of SSVEP-BCI controlled soft robotic glove in post-stroke hand function rehabilitation.
[Abstract] Upper extremity self-efficacy correlates with daily hand-use of individuals with high functional capacity post-stroke
Posted by Kostas Pantremenos in Paretic Hand on June 22, 2022
Abstract
Purpose
To understand the role of affected upper extremity (UE) self-efficacy for explaining daily-hand-use in individuals post-stroke. Specifically, to describe UE self-efficacy and to assess the associations between UE self-efficacy to UE motor and functional capacity and daily hand-use.
Materials and methods
This cross-sectional study included individuals post-stroke receiving rehabilitation with high UE functional capacity [Action Research Arm Test (ARAT) > 50]. The Rating of Everyday Arm-Use in the Community and Home (REACH) assessed perceived UE daily use and the Confidence in Arm and Hand Movement scale (CAHM) assessed UE self-efficacy. Functional capacity was assessed by the ARAT and the Fugl-Meyer-motor-assessment assessed motor impairment. Correlations between measures were assessed.
Results
Twenty-two individuals, aged 19–80, with high UE functional capacity [median (IQR) ARAT-56.5 (54–57)] and varying UE self-efficacy [median (IQR) CAHM-76.7 (58–84.4)], were included. UE self-efficacy was significantly correlated with the ARAT (rs = 0.53, p < 0.01) and REACH (rs = 0.51, p < 0.01) but ARAT was not significantly correlated with REACH.
Conclusions
UE self-efficacy is correlated with perceived daily hand-use in individuals with high functional capacity. Further research and a deeper understanding of the clinical implications of UE self-efficacy are warranted. UE self-efficacy should perhaps be assessed during rehabilitation.
- IMPLICATIONS FOR REHABILITATION
- Individuals with stroke with high affected upper extremity functional capacity do not necessarily use this hand for daily living.
- Upper extremity self-efficacy is correlated with perceived daily hand-use in individuals with high functional capacity; participants with higher upper extremity self-efficacy also reported more daily hand-use.
- Upper extremity self-efficacy seems to be upper extremity task or situation-specific.
- Upper extremity self-efficacy should be assessed during rehabilitation and the clinical implications of (low) upper extremity self-efficacy should be further researched.
[WEB] ReGrasp Bionic Glove is Now Available in the US
Posted by Kostas Pantremenos in Functional Electrical Stimulation (FES), Paretic Hand, Tele/Home Rehabilitation on May 17, 2022
Posted by Debbie Overman

ReGrasp Bionic Glove, a medical device designed to help patients speed hand rehabilitation following a stroke or injury, is now available in the United States for patients to use at home or in a clinical setting. It uses functional electrical stimulation (FES) technology, which researchers suggest could help improve hand function.
“Until now, rehabilitation gloves with FES technology have only been accessible to patients in a clinical setting,” said Dr. Rahul Samant, CEO of Rehabtronics. “Our research indicates that patients regain hand use faster when using ReGrasp for continuous therapy at home and functional use everywhere.”
A prescription from a physician or qualified therapist is required to purchase ReGrasp. The ReGrasp’s FES unit is easily programable by clinicians to set up functional home exercise programs (HEP) and to help patients use the glove as a functional device to perform daily tasks.
According to home health therapist Ashley Gatewood, OTR/L, ReGrasp motivates her patients to keep striving for independence.
“The ReGrasp provides patients with the opportunity to have functional rehabilitation at their fingertips in order to improve their independence and quality of life,” she says. “This device opens the door for patients to have access to advanced technology in their home, rather than just in a clinical setting.”
ReGrasp has a thin, fitted profile that is designed to be worn all day to help with day-to-day exercises. It is operated with a discrete wireless controller that sits securely behind the ear, allowing patients to control hand function using simple head movements.
[Source(s): Rehabtronics Inc, PR Newswire]
[WEB] Occupational and Physical Therapists See Promise in New Paired VNS Therapy for Stroke Recovery
Posted by Kostas Pantremenos in REHABILITATION on March 2, 2022
– Researchers and clinicians assert that the Vivistim® Paired VNS™ System is an adjunct intervention that improves outcomes of rehabilitation therapy for survivors of ischemic stroke
– FDA-approved Paired VNS Therapy generates 2-3 times more hand and arm function for stroke survivors than rehabilitation therapy alone
– The first commercial implantation of Vivistim is expected in the first half of 2022
AUSTIN, Texas, March 1, 2022 /PRNewswire/ — Rehabilitation therapy researchers and clinicians embrace the FDA-approved, first-of-its-kind Vivistim® Paired VNS™ System with a positive outlook as an effective, outcomes-based adjunct intervention for survivors of ischemic stroke.
Manufactured by MicroTransponder® Inc., a medical device company developing solutions to restore independence and dignity for people suffering from neurological conditions that impair sensory and motor function, the Vivistim System pairs vagus nerve stimulation with rehabilitation therapy to improve upper limb function for stroke survivors.

Occupational and Physical Therapists See Promise in New Paired VNS Therapy for Stroke Recovery
Results of MicroTransponder’s 108-person, multicenter, triple-blinded, randomized controlled pivotal clinical trial, published in The Lancet, show that the Vivistim System generates two to three times more hand and arm function for stroke survivors than rehabilitation therapy alone.
These results, along with the assertion of a paradigm shift in stroke rehabilitation, were presented by Teresa Jacobson Kimberley, Ph.D., PT, FAPTA, a professor at MGH Institute of Health Professions, and Steven L. Wolf, Ph.D., PT, FAPTA, FAHA, FASNR, a professor in the Division of Physical Therapy at Emory University School of Medicine, during the American Physical Therapy Association’s 2022 Combined Sections Meeting. Kimberley and Wolf, who led the Vivistim clinical trial at their respective institutions, facilitated a symposium titled “Applying the Evidence: The Emerging Role of Vagus Nerve Stimulation Paired with Stroke Rehabilitation.”
“The standard of care in rehabilitation therapy for stroke survivors has limited effect on the restitution of arm and hand function. The Vivistim VNS System paired with intense rehabilitation empowers occupational and physical therapists to enhance the benefits of the treatment they provide,” said Kimberley. “The evidence suggests that vagus nerve stimulation with rehabilitation therapy harnesses neurophysiology to enhance restitution.”
As Paired VNS Therapy garners more recognition for being an innovative, results-oriented intervention in stroke recovery, Wolf advocates for buy-in from rehabilitation specialists by underscoring that this new intervention is a complement to therapy, not a replacement.
“The challenge we have as neurorehabilitation professionals working with stroke survivors is changing the rate of recovery to make gains last longer before a patient’s movement ability plateaus,” said Wolf. “The use of vagus nerve stimulation may offer an opportunity to create such changes.”
According to occupational and physical therapists who participated in the clinical trial, the Vivistim System enables therapists to guide stroke survivors to significant improvements in upper limb mobility because of the innovativeness of the technology, the therapy’s unique in-clinic protocol and the system’s capability to be activated at home by the patient.
During Vivistim Therapy, a therapist will use a wireless transmitter that communicates with proprietary software to signal the implanted Vivistim device to deliver a gentle pulse to the vagus nerve while the stroke survivor performs a specific task, such as putting on a hat, brushing hair or cutting food. Through Vivistim’s at-home feature, stroke survivors can continue practicing rehabilitation exercises or practice routine tasks on their own by swiping the Vivistim magnet over the implant area.
Researchers believe that the simultaneous pairing of the rehabilitation exercise with vagus nerve stimulation releases neuromodulators that create or strengthen neural connections to improve upper limb function and increase the benefit of physical therapy.
“Paired VNS therapy is targeted to enhance neuroplasticity in the central nervous system of stroke survivors, so the exercises we conduct are more movement- and patient-specific,” said Nuray Yozbatiran, a physical therapist and research faculty member at the NeuroRecovery Research Center at TIRR Memorial Hermann and Department of Physical Medicine and Rehabilitation at UT Health McGovern Medical School.
Therapists evaluate their patient’s upper limb function during each Vivistim Therapy session to tailor the exercises around hand and arm functions that need the most improvement. According to Yozbatiran, patients reported that they felt challenged during the sessions and appreciated the intensity.
“Most of the patients I worked with during the clinical trial felt empowered with another chance at an intervention to improve their use and movement of the hemiplegic upper extremity. It motivated them to incorporate their hand and arm into tasks they had not recently performed,” said Komal Sahu, MPH, OTR/L, an occupational therapist at Emory Healthcare. “The follow-up with patients after completing the clinic sessions proved beneficial. All of the patients confirmed that they were continuing their 30-minute daily Vivistim at-home therapy and even asked for new and challenging activities to practice. It’s driven me to think of additional activities and exercises that will help my patients accomplish specific movements and goals.”
Even though the Vivistim System protocols are extensive, most therapists in the clinical trial report that it’s easy to integrate into their practice. During the clinical trials, 71% of therapists said it was easy or very easy to trigger the vagus nerve stimulation during therapy.
“The Vivistim System has helped me maintain an effective balance, delivering the VNS, guiding the patient through tasks, and only intervening to prevent the patient from doing compensatory movements,” said Isha Vora, MS, OTR/L, an acute care occupational therapist and Ph.D. student in the Brain Recovery Lab at MGH Institute of Health Professions.
Vora adds that Paired VNS Therapy can be effective for many survivors of ischemic stroke. The ideal candidates are probably survivors who are consistent with their follow-up appointments and who are motivated to participate in rehabilitation therapy. She’s seen patients who have previously been stagnant in therapy achieve significant improvement in their hand and arm function with Vivistim Therapy.
Clinical teams are currently identifying potential candidates for the Vivistim System, with the first commercial implantation of Vivistim expected in the first half of 2022. Rehabilitation specialists, physiatrists, neurologists and neurosurgeons interested in learning more can click here and assess if their patients are ideal candidates for the Vivistim System.
About MicroTransponder®, Inc.
MicroTransponder®, Inc. is a privately held, global medical device company based in Austin, Texas, committed to developing research-based neuroscience solutions. The company focuses on restoring independence and dignity for people suffering from neurological conditions that impair sensory and motor function. MicroTransponder’s FDA-approved Vivistim® Paired VNS™ System is a first-of-its-kind, clinically proven medical technology that generates two to three times more improvement in upper limb function than rehabilitation alone for stroke survivors after six weeks of in-clinic therapy. For more information, visit Vivistim.com.
Media Contact:
Julie Lopez
julie@microtransponder.com
SOURCE MicroTransponder
[BLOG POST] How to regain hand grasp and function
Posted by Kostas Pantremenos in Paretic Hand, Rehabilitation robotics on November 21, 2021
Spinal cord injury has been recorded in the hieroglyphs of Egypt. You can imagine the trauma that might have been sustained by workers of the great pyramids. This would be one of the first recorded industrial accidents. Pictorial evidence of urinary catheterization has been recorded by these early historians. It seems that spinal cord injury and other paralysis have been with us since the dawn of mankind.
Life after a spinal cord injury can sometimes feel a little hopeless because you have to rely on someone else for everything, even simple everyday tasks like feeding yourself or brushing your teeth. Although modern medicine has not yet found a way to cure paralysis, modern technology is starting to bridge the gap.
Table of contents
- How to adapt on your daily life
- Functional devices assist with everyday tasks
- Neomano: Regain hand function and independence
How to adapt on your daily life
More than one third of spinal cord injury survivors sustain an injury that causes damage to the spinal cord in the cervical region and results in tetraplegia. Most people with tetraplegia remain wheelchair-dependent and reliant on others for physical care. Limited hand and upper limb function is often more disabling and of greater importance to them than their inability to walk. Even modest improvements in hand function can have life-changing implications. For example, a small amount of finger movement enables a person with tetraplegia to use a keyboard, press a switch, scratch the face and turn the page of a book. The ability to do these simple tasks reduces dependency on others, improves potential for employment and enhances quality of life. Expanding these activities could be the aim of rehabilitation.
Functional Devices Assist with Everyday Tasks
Over the years there have been many functional splints and devices created to assist people with everyday tasks. One of the most commonly used functional devices is called a universal cuff. A universal cuff can be used in a variety of ways such as to hold a feeding utensil, tooth brush, or makeup brush, etc. Depending on the level of the spinal cord injury, one may require a wrist support splint along with the universal cuff or a mobile arm support which will provide a gravity eliminated position for the upper extremity, allowing active movement while utilizing less muscle strength.
Another common practice is utilizing foam to build up objects such as feeding utensils, tooth brush, or writing utensils. If someone needs a little more support for writing they may be recommended a functional writing splint such as a figure eight splint or a Wanchik Writer splint.
There have been many other devices and custom splints created in order to perform fun activities such as gardening, fishing and painting.
NeoMano: Regain Hand Function and Independence
Soft robotics is an emerging discipline that combines the classical principles of robotics with soft materials and could provide a new class of active assistive devices. Neofect has created a soft robotic assistive device called NeoMano that helps with hand motions in order to give people back their hand function and independence while only requiring one device. NeoMano is a wearable robotic glove that assists with the grasp and release of objects. The glove is a partial-glove design that enables the thumb, pointer and middle finger to perform grasp and release motions.
- Shop now – Neofect Shop
Actuated by the motor and pulley, the wireless remote control enables the grip and release of the index & middle finger. When activated, the Grip button flexes the fingers to provide a gripping gesture. The Release button loosens the wires, allowing the hand to return to its original neutral position. The wire is highly elastic, which helps maintain wire integrity despite repetitive winding and loosening.
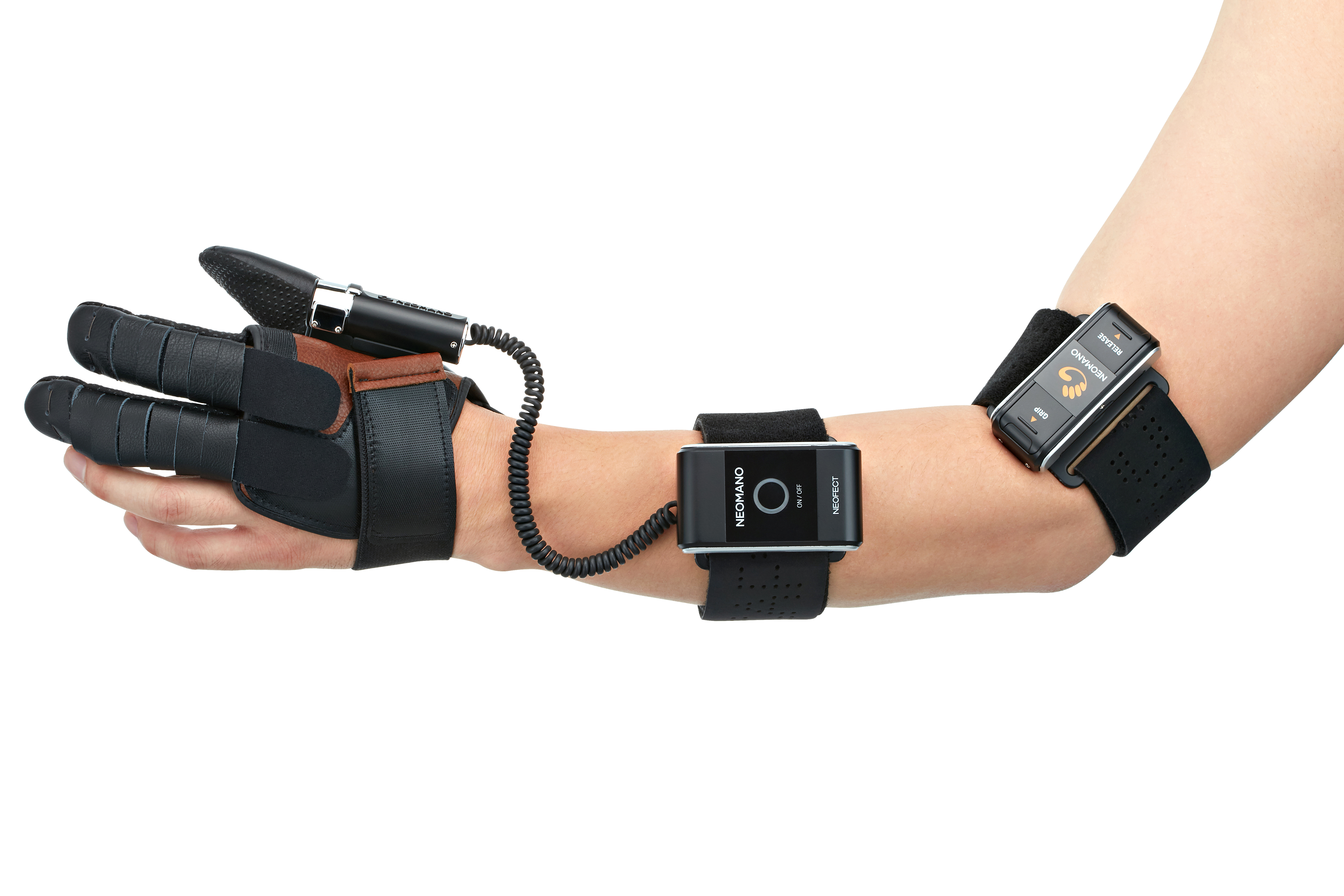
NeoMano can assist people with everyday tasks such as feeding, writing, exercising, and daily grooming tasks. People have even rediscovered old hobbies with the use of NeoMano, like golfing and photography!
[Abstract] Occupational therapists’ evaluation of the perceived usability and utility of wearable soft robotic exoskeleton gloves for hand function rehabilitation following a stroke
Posted by Kostas Pantremenos in Paretic Hand, REHABILITATION, Rehabilitation robotics on July 5, 2021
Abstract
Purpose
To evaluate the perceived usability and utility of using a soft robotic glove to rehabilitate hand function following a stroke.
Methods
A convergent parallel mixed-methods design was used to consult a convenience sample of 14 experienced occupational therapists (OTs) practicing within a specialised stroke rehabilitation program. All OTs participated in one 60-to-90-minute individual consultation during which the attributes of a recently-developed soft robotic glove (ExoGlove) were presented before they could test it on themselves. After this consultation, OTs completed the System Usability Scale (SUS) questionnaire and answered open-ended questions focussing on the usability and utility of soft robotic gloves framed according to the Unified Theory of Acceptance and Use of Technology (UTAUT).
Results
The OTs perceived the glove’s usability as being moderate-to-good on the SUS (median score= 63.75 on a scale of 100). Thematic analysis revealed the importance of specifically considering elements such as ease of use (e.g. simplicity and speed), cost, movement precision, durability, and safety, when developing soft robotic gloves such as the ExoGlove.
Conclusions
Engagement in a continuous improvement process is essential to maximise the perceived usability and utility of soft robotic gloves, particularly of the ExoGlove, through their final development phase before pilot testing their effects and effectiveness for post-stroke hand rehabilitation.
- Implications for rehabilitation
- All occupational therapists anticipate that a soft robotic glove such as the ExoGlove will allow them to increase treatment intensity and best aligns with principles of neuroplasticity.
- The clinical judgement and guidance of OTs, developed through practice, experience, and knowledge, remain essential to safely and efficiently exercise with a soft robotic glove.
- Achieving a balance between effort and performance expectancies is essential in developing and improving the functionality of soft robotic gloves, as with each additional functionality comes new challenges that impact its successful transition to a clinical setting.
